ORDER UTILITY
Fill out the fields below to receive your selected utility
[contact-form-7 404 "Not Found"]CareOptimize works directly with CareMax Medical Centers, seven full-risk, full-service Medicare Advantage facilities in South Florida. All provide a full spectrum of medical services, including transportation (fleet of 50 vans) and home visits. Because these centers are full-risk, it is imperative CareOptimize monitor each center carefully to ensure CareMax centers remain successful value-based operations. To help do this, they have come up with a suite of templates for physicians and coders to work together at point-of-care not only to make the most beneficial coding decisions, but also to simplify the process.
Managing MA members in comparison to FFS
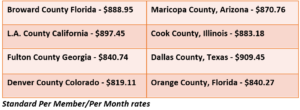
Medicare Advantage pays a capitated amount per beneficiary and focuses on proactive preventative care and early intervention. Care coordination and innovation are incentivized, and a risk adjustment model is used for patient differences. A comparison chart on cap rates per member per month illustrates how the MA contract rate fluctuates and how it might benefit practices.
Accurate HCC coding provides accurate RAF scores, and that accuracy reflects how well codes have been documented at point-of-care. Most CareMax members are joined with HealthSun, a large Medicare Advantage payer with a coveted 5-star rating from CMS. If HEDIS scores are managed well, HealthSun maintains their 5-star rating, which triggers a 5% bonus in addition to the base per patient per month payment.
By offering providers and payers accurate information, CareOptimize has been able to boost CareMax Medicare Advantage premiums. When Medicare Advantage is managed through accurate HCC coding, etc., even more funds can be generated.
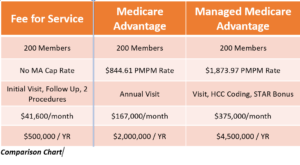
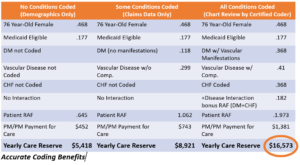
To maximize our systems and take advantage of the Medicare Advantage model, we created a system at point-of-care for physicians to ascertain exactly what they need for accurate coding. This system tracks HCC drop-offs and suspected and overdue codes. The coding review process between provider and coder was streamlined, so coding opportunities would be caught before claim creation. We wanted to back all of this up with aligned workflows in the EHR, so we designed templates to do just that.
The pre-audit process lets providers know there is a set number of patients for the next day. A pre-audit review is generated, which includes suggested codes by coders based on holistic evidence. The physician can see and review the information at point-of-care, including codes, diagnosis descriptions, and status of patient (new or not) in their daily assessments. They can accept the code as is if they feel it’s valid or choose no evidence of disease right there, and go on with their notes. Simplifying the coding process benefits both provider and payer, giving crucial information at point-of-care to be generated, allowing for much more accurate results.